top of page

Knee Pain
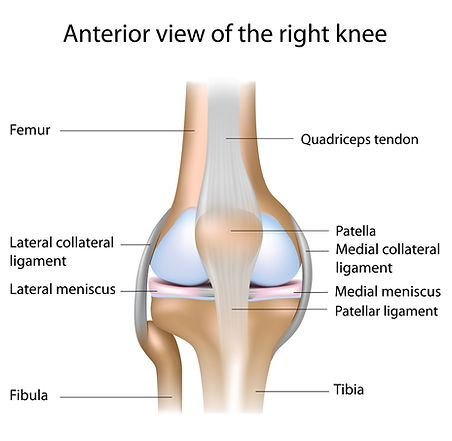
The knee joint is a hinge joint with strong ligaments between the thigh and shin bones. Smooth cartilage covers the end of bones to reduce friction. There are also two extra pieces of thick cartilage called menisci which act as shock absorbers.
The knee ligaments and capsule (the bag that surrounds the joint), prevent the bones moving in the wrong direction or dislocating. The thigh muscles (quadriceps) also help to hold the knee joint in place and produce movement.
Problems with knee joints are common. See below for information on conditions / self help.
Common causes of knee pain
What is Knee Osteoarthritis?
Osteoarthritis (OA) is a common condition which can affect any joint, but commonly the knee. The cartilage which protects the surface of your joints get worn/damaged which causes friction and prevents the joint from moving smoothly.
The joint can become swollen and inflamed, the joint can change shape and the muscles can feel weaker.
The knee joint is made up of three main compartments, the medial tibiofemoral joint (inner aspect of the knee), the lateral tibiofemoral joint (outside aspect of the knee) and the patellofemoral joint (where the knee cap moves across the front of the femur).
Sometimes knee osteoarthritis affects one compartment of the joint rather than all three.
Causes:
• Normal age-related changes.
• Previous injury to the area.
• Repetitive activity/physical job.
• Family history.
• High Body Mass Index.
• It is more common in people over the age of 50.
Symptoms:
• Early morning stiffness in the knee, in the morning for 30 minutes or more.
• Instability.
• Swelling.
• Reduced movement in the knee, particularly bending the knee.
• Reduced ability to complete activities of daily living.
• Pain in the knee.
• Putting weight through the affected knee.
Treatment:
Most commonly a physiotherapist will be able to make a diagnosis of knee osteoarthritis through an assessment of your knee and talking to you about your symptoms.
Sometimes it may be necessary to complete an X-RAY of the knee, however this dependent on your duration of symptoms and/or if you have trialled physiotherapy rehabilitation with limited improvement.
The most common methods of treatment will include:
• Physical activity.
• Weight loss.
• Strengthening exercises.
• Advice/education regarding osteoarthritis.
• Pain relief - please speak to your GP regarding medication.
If you fail to respond to physiotherapy treatment, sometimes the following options may be appropriate:
• Steroid injection into the knee joint.
• Orthopaedic opinion if you have limited improvement with conservative management.
Exercises:
Level 1:
Start off with these level 1 exercises for your knee, if you need help - please contact a health professional. These exercises should not be painful however they may be more sore to start with and get easier the more you do them.
Pick a couple of exercises to start with and add more as you feel able.
• Straight leg raise
https://video.wixstatic.com/video/e7d8af_3c50df4cb6624500b96a0d3b9ed1a83e/1080p/mp4/file.mp4
In sitting with your legs out in front, lift your leg up towards the ceiling in a straight position and lower back down. Try lift your heel at the same time as your knee.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Inner range quads
https://video.wixstatic.com/video/e7d8af_a45d5c7df9ec4542aa88b1a2f0edb67e/1080p/mp4/file.mp4
In sitting with your legs out in front, place a pillow underneath your knee, tense your thigh muscles and lift your heel off the floor. Slowly lower your heel back down to the position you started in.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Double leg Glute bridge
https://video.wixstatic.com/video/e7d8af_16cb92892ff2495fa0ab0b5d994c8b81/1080p/mp4/file.mp4
Laying on your back, place your feet hip-width apart on the floor and place your hands across your chest. Squeeze your bottom and push through your heels to lift your bottom off the floor. If you are struggling with balance, place your hands on the bed either side of you.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Squat
https://video.wixstatic.com/video/e7d8af_81069ce1e05949199f8178bb7c1899a7/1080p/mp4/file.mp4
In standing, place feet hip-width apart, bend your knees and push your bottom backwards to lower yourself down. Keep your chest facing forward and look forward. Push through yours legs to stand back up and squeeze your bottom at the top of the movement.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Sit to stand
https://video.wixstatic.com/video/e7d8af_f90f513f820b446089e25028cef2a46e/1080p/mp4/file.mp4
In sitting, place your hands across your chest. Place your feet hip width apart, lean forward and push through your legs to stand up. Try avoid using your hands to push to stand and use your legs to stand up. Sit back down, bending your knees and pushing your bottom back to the chair.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
Level 2:
If you feel you have progressed with the level 1 exercises and would like some harder exercises, please have a go at the level 2 exercises. These exercises should not be painful however they may be more sore to start with and get easier the more you do them.
Pick a couple of exercises to start with and add more as you feel able.
• Lateral Step Down
https://video.wixstatic.com/video/e7d8af_e65eba67bf924ffbb8c5020212f95d92/1080p/mp4/file.mp4
Standing on a step on one leg, lower yourself down to the floor bending your knee. Skim your other foot off the floor and then push back up to standing using the opposite leg. If needed, hold onto a bannister to maintain balance.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Staggered Sit to Stand
https://video.wixstatic.com/video/e7d8af_0d1c55c836c44dc998a5196d82a7a841/1080p/mp4/file.mp4
In sitting, place your hands across your chest. Place your feet hip width apart, with one foot slightly further in front than the other, lean forward and push through your legs to stand up. Try avoid using your hands to push to stand. Sit back down, bending your knees and pushing your bottom back into to the chair. If you can do this, progress to the ‘single leg sit to stand’.
The lower the chair height, the harder this exercise will be. You could place a pillow on the chair seat to make it easier.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Single Leg Sit to stand
https://video.wixstatic.com/video/e7d8af_2caa4874bd72454da65f30c6fffe51ab/1080p/mp4/file.mp4
In sitting, place your hands across your chest. Place your feet hip width apart, with one foot on the floor and one foot off the floor out in front, lean forward and push through your leg to stand up. Try avoid using your hands to push to stand up, Sit back down, bending your knee and pushing your bottom back into the chair. The lower the chair height, the harder this exercise will be. You could place a pillow on the chair seat to make it easier.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Staggered Glute Bridge
https://video.wixstatic.com/video/e7d8af_ce61b64491e84a49811f927d83553d8d/1080p/mp4/file.mp4
Laying on your back, place your feet hip-width apart and place your hands across your chest. Bend your knees and place one foot slightly further away than the other foot. Squeeze your bottom and push through your heels to lift your bottom off the floor. If you are struggling with balance, place your hands on the bed either side of you. The further one foot is away from you, the harder this exercise will be.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
• Single Leg Glute Bridge
https://video.wixstatic.com/video/e7d8af_0518ce2144ee440e8758cfacac8de23e/1080p/mp4/file.mp4
Laying on your back, place your feet hip-width apart and place your hands across your chest. Bend one knee with the foot on the floor and place one leg off the floor. Squeeze your bottom and push through your foot that is on the floor to lift your whole bottom off the floor. If you are struggling with balance, place your hands on the bed either side of you.
Complete 3 sets of 10 repetitions (3x10) - 2-3 times a week.
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
• Arthritis UK, have also developed an exercise page where you can follow step by step exercises to help with your Knee Osteoarthritis. Please click the link below: https://www.arthritis-uk.org/information-and-support/living-with-arthritis/health-and-wellbeing/exercising-with-arthritis/exercises-for-healthy-joints/exercises-for-the-knees/(https://www.arthritis-uk.org/information-and-support/living-with-arthritis/health-and-wellbeing/exercising-with-arthritis/exercises-for-healthy-joints/exercises-for-the-knees/)
• Versus Arthritis OA Knee Booklet
https://www.versusarthritis.org/media/24020/osteoarthritis-of-the-knee-august2021.pdf (https://www.versusarthritis.org/media/24020/osteoarthritis-of-the-knee-august2021.pdf)
• National Institute for Health and Care Excellence - Guidelines for knee osteoarthritis. Please click the link here: Recommendations | Osteoarthritis in over 16s: diagnosis and management | Guidance | NICE (https://www.nice.org.uk/guidance/ng226/chapter/Recommendations#non-pharmacological-management)
• Live Well with pain website. Please click the link here: https://livewellwithpain.co.uk/(https://livewellwithpain.co.uk/)
Last reviewed April 2026. To be reviewed April 2027.
What is an acute meniscus injury?
There are two menisci in each knee. They are shock absorbing cartilages and sit between your shin and thigh bone. One on the inside and one on the outside of your knee. The meniscus is needed for joint stability and lubrication.
A acute meniscus injury is caused usually by a tear or irritation in the meniscus tissue. Because the meniscus has poor blood supply, rehabilitation including strengthening, is very important for healing.
Generally those who are younger, will have meniscus pain related to an injury.
If your pain started after a minor/no injury, it is likely your pain is related to degenerative meniscus. For more information, please see information on degenerative meniscus pain page.
Causes:
• Twisting the knee whilst putting weight through it, most commonly in football/netball.
• A direct impact on the knee.
Symptoms:
• Pain around the knee.
• Swelling around the knee.
• Clicking.
• Lack of knee movement and reduced ability to complete activities of daily living.
• Locking (the joint becomes stuck in one position).
• Giving way.
Treatment:
Most commonly a physiotherapist will be able to make a diagnosis of an acute meniscus tear through an assessment of your knee and talking to you about your symptoms.
Things you can do to help yourself in the first week following a meniscus injury to your knee:
• Protection: During the first few days after an injury, you should rest the injured joint. After 72 hours, gentle movement can be started. If walking is difficult or painful, a stick or crutch may help.
• Although it might be painful, it is important to maintain movement in your knee to avoid stiffness. Placing no weight through the joint at all is rarely useful.
• Ice: Applying ice with gentle compression using a bandage may help with pain relief and reducing swelling around your knee.
• Elevation: Placing the knee higher than your hip whilst lying or sitting will help the swelling reduce.
• Use of over the counter pain relief if necessary to enable to keep mobile. (Speak to your local Pharmacist if you are unsure about what you can take).
The most common methods of treatment will include:
• Physical activity.
• Weight loss.
• Strengthening exercises.
• Advice/education regarding meniscus injuries.
• Pain relief - such as anti-inflammatory medication - please speak to your GP regarding medication.
If you fail to respond to physiotherapy treatment, sometimes the following options may be appropriate:
• Steroid injection into the knee joint.
• Orthopaedic opinion if you have limited improvement with conservative management.
Sometimes it may be necessary to complete an X-RAY of the knee, however this dependent on your duration of symptoms and/or if you have trialled physiotherapy rehabilitation with limited improvement.
If an X-RAY shows no degenerative changes such as osteoarthritis, it may be appropriate to complete an MRI for surgical planning. Most symptoms will settle down with time, exercise and rehabilitation, therefore these options are recommended as first line treatment.
In most cases, meniscal tears can be managed without surgery.
Exercises:
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
Last Reviewed Jan 2026. To be reviewed Jan 2027.
What is Degenerative Meniscus Pain?
There are two menisci in each knee. They are shock absorbing cartilages and sit between your shin and thigh bone. One on the inside and one on the outside of your knee. The meniscus is needed for joint stability and lubrication. Because the meniscus has poor blood supply, rehabilitation including strengthening, is very important for healing.
Degenerative meniscus tear/irritation is generally related to pain that started after a minor injury or no injury. Like grey hairs and wrinkles, they are a normal part of the ageing process, as the meniscus tissues change and become more vulnerable to injury. Degenerative meniscus tears are often associated with knee osteoarthritis. They most commonly occur over the age of 35.
More than a third of people over the age of 50 will have one – but they do not all have symptoms. Sometimes you may have degenerative meniscus but have no pain.
Most degenerative meniscal tears don’t cause symptoms and are just as likely to be present in people with and without knee pain. The pain may fluctuate and resolve with time
Causes:
• Usually from a slow and quiet onset where you may have no or a very minor injury (Eg. stumble, twisting).
The following reasons increase your risk of a degenerative meniscus tear:
• Being male.
• Work related kneeling.
• Squatting.
• Sitting for long periods.
• Stair climbing.
• Having a body mass index over 25.
Symptoms:
• Pain around the knee (usually the inside aspect or the outside aspect).
• Swelling around the knee (usually a occurring a few hours after the injury).
• Clicking.
• Lack of knee movement and reduced ability to complete activities of daily living.
• Locking (the joint becomes stuck in one position).
• Giving way.
Treatment:
Most commonly a physiotherapist will be able to make a diagnosis of degenerative meniscus pain through an assessment of your knee and talking to you about your symptoms.
Things you can do to help yourself in the first week following a meniscus injury to your knee:
• Protection: During the first few days after an injury, you should rest the injured joint. After 72 hours, gentle movement can be started. If walking is difficult or painful, a stick or crutch may help.
• Although it might be painful, it is important to maintain movement in your knee to avoid stiffness. Placing no weight through the joint at all is rarely useful. Using some walking aids in the short term may be helpful to offload some weight through the knee.
• Ice: Applying ice with gentle compression using a bandage may help with pain relief and reducing swelling around your knee.
• Elevation: Placing the knee higher than your hip whilst lying or sitting will help the swelling reduce.
• Use of over the counter pain relief if necessary to enable to keep mobile. (Speak to your local Pharmacist if you are unsure about what you can take).
The most common methods of treatment generally 1 week post injury will include:
• Physical activity.
• Weight loss.
• Strengthening exercises.
• Advice/education regarding meniscus injuries.
• Pain relief - please speak to your GP regarding medication. In the early stages 1-3 weeks, anti-inflammatory medication is not recommended however beyond this time frame, it may help to ease your symptoms.
If you fail to respond to physiotherapy treatment, sometimes the following options may be appropriate:
• Steroid injection into the knee joint.
• Orthopaedic opinion, if you have limited improvement with conservative management.
Do I need a scan?
Sometimes it may be necessary to complete an X-RAY of the knee to rule out other causes and determine the severity of osteoarthritis. However this is dependent on your duration of symptoms and/or if you have trialled physiotherapy rehabilitation with limited improvement.
Guidelines suggest unless you have a traumatic injury to the knee or are suddenly unable to straighten your knee or a serious cause of pain is suspected; MRI scans are usually not needed and it can lead to unnecessary treatment.
Do I need surgery?
Surgery is not always needed for degenerative meniscal tears because, unlike sudden injuries in younger people, these tears usually happen as part of the normal ageing process. Many people find that with simple treatments like exercise therapy, activity modification, and pain relief, their symptoms improve just as much as they would with an operation. In fact, research has shown that physiotherapy can be just as effective as surgery for many patients, without the risks or recovery time that come with an operation. That’s why surgeons often recommend trying non-surgical options first.
Exercises:
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
Last Reviewed Jan 2026. To be reviewed Jan 2027.
What is an Anterior Cruciate Ligament tear?
The anterior cruciate ligament (ACL) is a strong band of tissue inside your knee joint. It's main role is to help control the stability of our knee and prevent unnecessary movement. Tearing this ligament can result in pain, swelling and difficulty in trusting the knee to help us walk and run.
As a result of this injury, sometimes the meniscus may be also be torn. For more information on mensical injuries please click here (https://www.harrogatehealthhub.co.uk/knee-pain)and select the drop down for "Acute Meniscal Injuries".
Causes:
• Rapid movement of the knee moving inwards or outwards whilst the foot is planted on the floor.
• The knee being forced backwards (also known as hyperextension).
• Direct blow to the knee.
• Landing on bent a knee.
• Sudden change of direction.
• Deceleration whilst running.
Most injuries to the ACL occur as a result of a twisting injury when playing sports such as rugby, tennis, skiing, netball and football.
Symptoms:
• Popping sensation at the time of injury.
• Giving way of the knee.
• Immediate swelling of the knee.
• Unable to carry on playing or unable to weight bear through the knee.
• Bruising may be present following the injury.
• Clicking or catching sensations.
Treatment:
To diagnose a ACL tear, you may be seen by a Physiotherapist or an Orthopaedic doctor. They will talk to your about how the injury happened, give the knee a physical examination and you may be refereed for an MRI scan of the knee.
If you have torn your ACL, the team at the hospital will discuss with you the options.
• The first option would be to try non-surgical rehabilitation. In some patients, this can work very well and although it can take time they can make a very good recovery.
• The second option would be to have the ACL surgically repaired. This is done via an arthroscopy (key hole surgery). You can find out more about this by clicking the link below:
Things you can do to help yourself in the first few weeks following a suspected ACL injury to your knee:
• Protection: During the first few days after an injury, you should rest the injured joint. After 72 hours, gentle movement can be started. If walking is difficult or painful, a stick or crutch may help.
• Although it might be painful, it is important to maintain movement in your knee to avoid stiffness. Placing no weight through the joint at all is rarely useful.
• Ice: Applying ice with gentle compression using a bandage may help with pain relief and reducing swelling around your knee.
• Elevation: Placing the knee higher than your hip whilst lying or sitting will help the swelling reduce.
• Use of over the counter pain relief if necessary to enable to keep mobile. (Speak to your local Pharmacist if you are unsure about what you can take).
The most common methods of treatment will include:
• Physical activity.
• Strengthening exercises.
• Advice/education regarding ACL injuries.
• Pain relief - such as anti-inflammatory medication - please speak to your GP regarding medication.
Exercises:
Please watch this video for early stage ACL rehabilitation:
https://video.wixstatic.com/video/e7d8af_135d0d4a195545d594c2c0ab664e3dc5/720p/mp4/file.mp4
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
Last reviewed February 2026. To be reviewed February 2027.
What are medial collateral ligament and lateral collateral ligament injuries?
The knee ligaments give the bones of the knee stability, by helping to keep them together. There are two main sets of ligaments in your knee. The collaterals, which run down the sides of your knee and the cruciate ligaments, that are inside the knee.
Lateral Collateral Ligament (LCL):
The lateral collateral ligament is located on the outside of the knee.
Medial Collateral Ligament (MCL):
The medial collateral ligament is on the inside of your knee.
Causes:
• Rapid movement of the knee moving inwards or outwards whilst the foot is planted on the floor.
• The knee being forced backwards (also known as hyperextension).
• Direct blow to the knee.
• Landing on bent a knee.
• Sudden change of direction.
• Deceleration whilst running.
A MCL Injury of the knee is usually a result of a jumping or twisting injury or falling on a bent knee e.g a fall in skiing or when being tackled.
However, a number of these injuries are not related to sport. They can be from a sudden twisting of the knee or repeated trauma to the knee; putting stress on the ligament which can change the elasticity of the ligament.
Symptoms:
• Popping sensation at the time of injury.
• Giving way of the knee.
• Immediate swelling of the knee.
• Unable to carry on playing or unable to weight bear through the knee.
• Bruising may be present following the injury.
• Clicking or catching sensations.
Treatment:
Following a traumatic knee injury, you may be seen by a Physiotherapist or an Orthopaedic doctor. They will talk to your about how the injury happened, give the knee a physical examination and you may be referred for an MRI scan of the knee.
Things you can do to help yourself in the first few weeks following a suspected MCL/LCL injury to your knee:
• Protection: During the first few days after an injury, you should rest the injured joint. After 72 hours, gentle movement can be started. If walking is difficult or painful, a stick or crutch may help.
• Although it might be painful, it is important to maintain movement in your knee to avoid stiffness. Placing no weight through the joint at all is rarely useful.
• Ice: Applying ice with gentle compression using a bandage may help with pain relief and reducing swelling around your knee.
• Elevation: Placing the knee higher than your hip whilst lying or sitting will help the swelling reduce.
• Use of over the counter pain relief if necessary to enable to keep mobile. (Speak to your local Pharmacist if you are unsure about what you can take).
The most common methods of treatment will include:
• Physical activity.
• Strengthening exercises.
• Advice/education regarding MCL/LCL injuries.
• Pain relief - such as anti-inflammatory medication - please speak to your GP regarding medication.
Exercises:
Click below to download MCL exercise sheet
Level 1 - Early stage exercises for a MCL injury
Level 2 - Mid / Late stage exercises for a MCL injury
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
Last reviewed March 2026. To be reviewed March 2027.
What is a patella dislocation?
Patella (Kneecap) dislocations are a common injury.
The Patella usually moves within a grove (Trochlea) and sometimes it comes out of that grove causing the kneecap to dislocate this can also cause damage to the muscles and ligaments around the knee.
Most commonly, the patella relocate its self but in some cases may need a health care professional to help.
As a result of a dislocation sometimes you may experience muscle or ligament injury which may contribute to long term symptoms.
Causes:
• Direct blow to the knee
• Sports injury
• Hypermobility
• Being a young female is a risk factor.
Symptoms:
• Clicking/catching sensation
• Giving way of the knee
• Swelling
• Pain
• Weakness
• Reduced ability to move the knee through full movement
• Apprehension to move the knee
Treatment:
Firstly, the kneecap must be relocated; in some cases you might be given a brace to wear, this will only be for a short period.
Things you can do to help yourself in the first week following a patella dislocation injury to your knee:
• Protection: During the first few days after an injury, you should rest the injured joint. After 72 hours, gentle movement can be started. If walking is difficult or painful, a stick or crutch may help.
• Although it might be painful, it is important to maintain movement in your knee to avoid stiffness. Placing no weight through the joint at all is rarely useful.
• Ice: Applying ice with gentle compression using a bandage may help with pain relief and reducing swelling around your knee.
• Elevation: Placing the knee higher than your hip whilst lying or sitting will help the swelling reduce.
• Use of over the counter pain relief if necessary to enable to keep mobile. (Speak to your local Pharmacist if you are unsure about what you can take).
The most common methods of treatment will include:
• Physical activity.
• Weight loss.
• Strengthening exercises.
• Advice/education regarding patella injuries.
• Pain relief - such as anti-inflammatory medication - please speak to your GP regarding medication.
If you fail to respond to physiotherapy treatment, sometimes the following options may be appropriate:
• Orthopaedic opinion if you have limited improvement with conservative management.
Sometimes it may be necessary to complete an X-RAY of the knee, however this dependent on your duration of symptoms and/or if you have trialled physiotherapy rehabilitation with limited improvement.
Exercises:
Click the links below for exercises:
Level 1 - Early stages:
Level 2 - Mid-Late stages:
Further resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
Last reviewed March 2026. To be reviewed March 2027.
The Patellofemoral joint (PFJ) is the joint between the knee cap and the thigh bone. Problems with the PFJ can lead to pain anywhere around the knee.
Causes:
1. Too much loading too quickly eg. Hill walking on holidays, or taking up new sports. Repetitive bending and kneeling can make it worse.
2. Anything that can affect the knee cap sliding correctly e.g flat feet, knocked knees etc
3. Injury e.g falls
Symptoms:
• Does not usually come on with trauma. More common after activity you have not done much of before....e.g walking, stairs or cycling.
• Pain is usually to the front of the knee.
• The pain may get worse the more you walk or go up or down stairs
• It is more common in people over the age of 30
• More common in overweight people.
• A diagnosis is made by your clinical history. A scan would not normally show very much
Treatment:
1. Exercise helps to keep the muscles strong so they will support the joint and help improve your symptoms.
2. Stretching the muscles will also help. Keep thigh, calf and hamstrings muscles as flexible as possible (see below).
3. Avoid sustained activity/positions e.g sitting for long periods/ doing repetitive exercises as these can provoke the pain.
Exercises:
EXERCISES COMING SOON!
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
Last reviewed March 2026. To be reviewed March 2027.
What is Patella/quadriceps Tendinopathy?
COMING SOON!
Causes:
COMING SOON!
Symptoms:
COMING SOON!
Treatment:
COMING SOON!
Exercises:
COMING SOON!
Further Resources:
• Nuffield Joint Pain Programme - A six month programme which is designed to help you self-manage your joint pain, with access to Nuffield Facilities and lifestyle advice and exercise sessions. You can refer yourself. Please click the link here: https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme (https://www.nuffieldhealth.com/about-us/our-impact/healthy-life/joint-pain-programme)
• Active North Yorkshire - Healthy You - 12 week free weight loss programme and gym access. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/healthy-living/healthy-you (https://www.northyorks.gov.uk/healthy-living/healthy-you)
• Active North Yorkshire - Exercise Classes. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes (https://www.northyorks.gov.uk/active-north-yorkshire/exercise-classes)
• Active North Yorkshire - MSK Hub: The MSK Hub is a free 12 week programme to help support working people that have a reduced ability to work due to musculoskeletal joint pain. You can refer yourself. Please click the link here: https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions (https://www.northyorks.gov.uk/active-north-yorkshire/lifestyle-and-wellbeing-sessions/help-musculoskeletal-conditions)
Last reviewed March 2026. To be reviewed March 2027.
Please see the information below regarding different types of knee surgery:
Considering a knee replacment?


Considering ACL Reconstruction Surgery?
bottom of page

